Understanding the normal value of Po2 is important for anyone imply in respiratory physiology, critical care, or pulmonary medicine. Po2, or partial pressing of oxygen, is a fundamental measurement that indicates the amount of oxygen dissolved in the blood. This value is essential for valuate respiratory mapping, diagnosing respiratory disorders, and monitoring the effectiveness of oxygen therapy. This blog post will delve into the significance of Po2, its normal range, factors touch it, and how it is measure.
What is Po2?
Po2, or partial press of oxygen, refers to the pressing exerted by oxygen molecules in a gas potpourri. In the context of human physiology, Po2 is frequently used to describe the amount of oxygen resolve in the blood. This measurement is critical for interpret how well the lungs are functioning and how effectively oxygen is being delivered to the body s tissues.
Normal Value of Po2
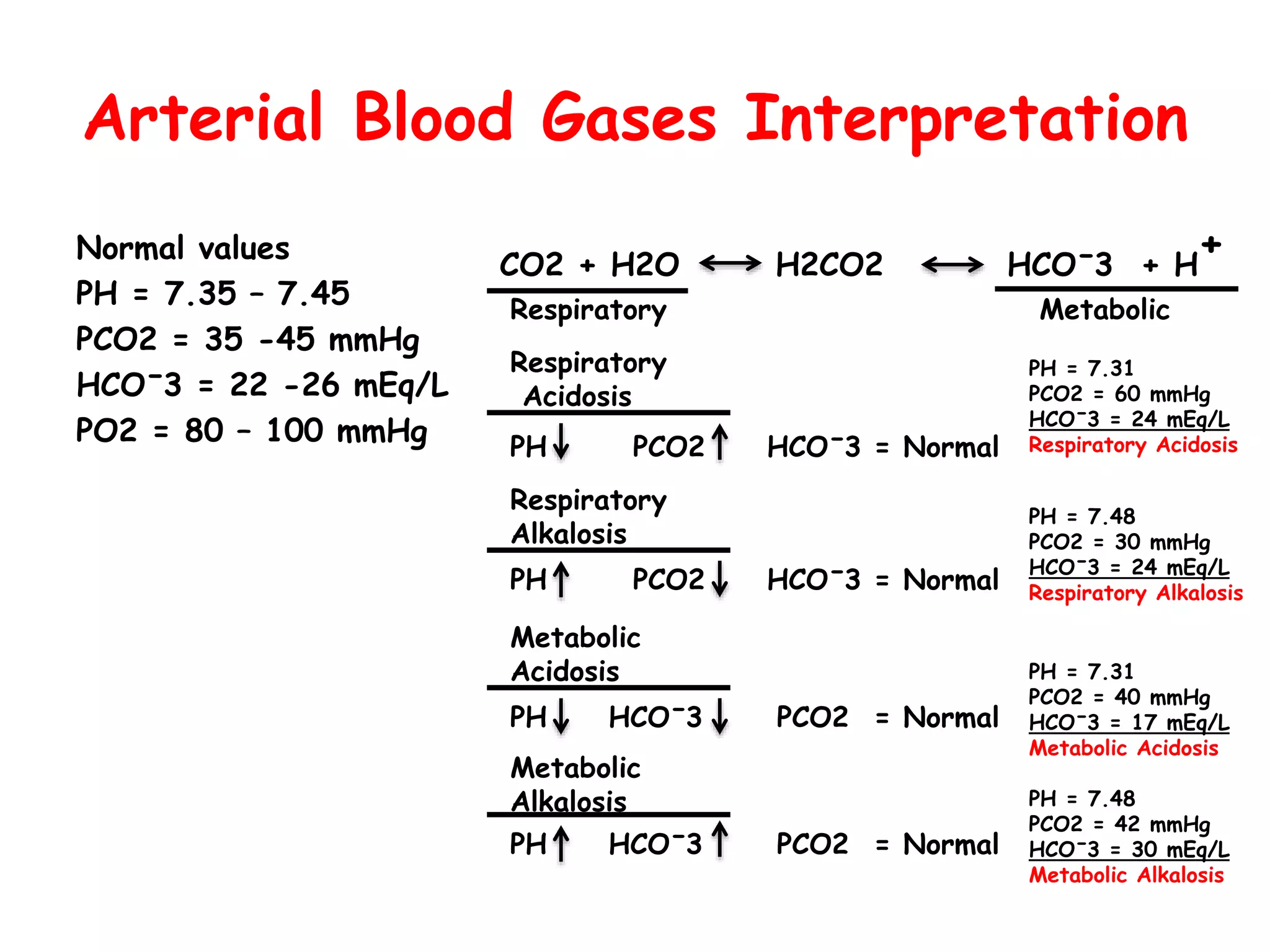
The normal value of Po2 in arterial blood (PaO2) typically ranges from 80 to 100 mmHg (millimeters of mercury) when respire room air at sea level. This range can vary slightly depending on the item-by-item s age, altitude, and overall health. for instance, in healthy adults at sea level, the normal PaO2 is unremarkably around 95 mmHg. However, notably that these values can alter with age and altitude.
Factors Affecting Po2
Several factors can influence the normal value of Po2. Understanding these factors is essential for render Po2 measurements accurately.
- Altitude: At higher altitudes, the atmospheric pressure is lower, which means there is less oxygen useable. This can leave to a decrease in Po2.
- Age: As people age, their lung role naturally declines, which can regard Po2 levels.
- Respiratory Diseases: Conditions such as continuing impeding pneumonic disease (COPD), asthma, and pneumonia can impair oxygen exchange in the lungs, starring to lower Po2 levels.
- Cardiovascular Health: Heart conditions that impact blood flow can also encroachment Po2 levels, as oxygenise blood may not be distributed expeditiously throughout the body.
- Oxygen Therapy: The administration of supplementary oxygen can increase Po2 levels, which is much necessary for patients with respiratory distress or other conditions that impair oxygenation.
Measuring Po2
Po2 is typically quantify using arterial blood gas (ABG) analysis. This routine involves line a sample of arterial blood, ordinarily from the radial artery in the wrist, and canvass it to set the fond pressures of oxygen and carbon dioxide, as well as the pH and bicarbonate levels. ABG analysis provides worthful info about a patient s respiratory and metabolic status.
Interpreting Po2 Levels
Interpreting Po2 levels involves equate the measure value to the normal value of Po2 and reckon the patient s clinical context. Here are some general guidelines for see Po2 levels:
- Normal Po2: A Po2 level within the normal range (80 100 mmHg) indicates that the lungs are functioning properly and that oxygen is being effectively delivered to the body s tissues.
- Low Po2 (Hypoxemia): A Po2 level below 80 mmHg suggests hypoxemia, which means there is not enough oxygen in the blood. This can be caused by various conditions, include respiratory diseases, heart failure, and anemia.
- High Po2 (Hyperoxemia): A Po2 degree above 100 mmHg may point hyperoxemia, which can occur with the establishment of subsidiary oxygen or in certain aesculapian conditions. While high Po2 levels are generally not harmful in the short term, prolonged hyperoxemia can lead to oxygen toxicity.
Clinical Significance of Po2
The clinical significance of Po2 lies in its ability to cater insights into a patient s respiratory and cardiovascular health. Po2 measurements are used in various clinical settings, including:
- Critical Care: In intensive care units (ICUs), Po2 levels are nearly monitored to ensure that critically ill patients are receiving adequate oxygenation. This is particularly important for patients with respiratory failure, sepsis, or other life jeopardise conditions.
- Pulmonary Medicine: Po2 measurements are essential for diagnosing and managing respiratory diseases such as COPD, asthma, and pulmonary fibrosis. They help clinicians assess the severity of the disease and the effectiveness of treatment.
- Anesthesiology: During surgery, Po2 levels are monitored to ensure that the patient is obtain adequate oxygenation and to detect any potential complications betimes.
- High Altitude Medicine: At high altitudes, the normal value of Po2 decreases due to the lower atmospheric press. Po2 measurements are used to assess the risk of altitude malady and to usher the use of supplementary oxygen.
Po2 and Oxygen Therapy
Oxygen therapy is a common intervention used to increase Po2 levels in patients with hypoxemia. The destination of oxygen therapy is to lift the Po2 to a level that ensures adequate oxygen delivery to the body s tissues. The amount of supplemental oxygen required depends on the severity of the hypoxemia and the patient s underlying condition.
Oxygen therapy can be deal through various methods, include:
- Nasal Cannula: A adenoidal cannula delivers low flow oxygen through the nostrils. It is commonly used for patients with mild to check hypoxemia.
- Face Mask: A face mask can deliver higher concentrations of oxygen and is often used for patients with more severe hypoxemia.
- Non Invasive Ventilation (NIV): NIV, such as continuous confident airway pressing (CPAP) or bilevel plus airway pressure (BiPAP), can be used to deliver oxygen and endorse breathing in patients with respiratory failure.
- Mechanical Ventilation: In severe cases, mechanical ventilation may be necessitate to support suspire and ensure adequate oxygenation.
Monitoring Po2 Levels
Regular supervise of Po2 levels is essential for grapple patients with respiratory conditions. This can be done through:
- Arterial Blood Gas (ABG) Analysis: ABG analysis provides a unmediated measurement of Po2 and is the gold standard for assessing oxygenation status.
- Pulse Oximetry: Pulse oximetry is a non incursive method that estimates the oxygen impregnation (SpO2) in the blood. While it does not directly measure Po2, it provides a quick and easy way to monitor oxygenation status.
- Capnography: Capnography measures the concentration of carbon dioxide in exhaled breath and can provide indirect information about ventilation and oxygenation status.
Note: While pulse oximetry is a commodious and non incursive method for supervise oxygenation, it should not replace ABG analysis in critical care settings. Pulse oximetry may not accurately reflect Po2 levels in patients with certain conditions, such as carbon monoxide poisoning or severe anemia.
Po2 and Altitude
As mentioned earlier, altitude can significantly affect the normal value of Po2. At higher altitudes, the atmospheric pressure is lower, which means there is less oxygen available for breathe. This can lead to a decrease in Po2 levels and an increase risk of altitude nausea.
Altitude sickness, also known as acute mountain sickness (AMS), is a common stipulation that occurs when the body is not acclimate to the lower oxygen levels at eminent altitudes. Symptoms of AMS include headache, nausea, dizziness, and fatigue. In severe cases, it can progress to high altitude pulmonary edema (HAPE) or high altitude intellectual edema (HACE), which are life menace conditions.
To prevent altitude sickness, it is significant to acclimate gradually to higher altitudes and to monitor Po2 levels. Supplemental oxygen may be necessary for individuals who are especially susceptible to altitude malady or who are ascend to very high altitudes.
Po2 and Exercise
During exercise, the body s demand for oxygen increases, and Po2 levels can change consequently. In healthy individuals, the body is able to increase oxygen uptake and delivery to converge the increase demand. However, in individuals with respiratory or cardiovascular conditions, exercise may conduct to a decrease in Po2 levels, indicate impaired oxygenation.
Monitoring Po2 levels during do can provide valuable info about a patient's respiratory and cardiovascular role. This is especially important for individuals with conditions such as COPD, asthma, or heart failure, who may experience practise induced hypoxemia.
Exercise testing, such as a cardiorespiratory do test (CPET), can be used to assess Po2 levels during exercise and to judge the body's response to increased oxygen demand. This information can be used to guide treatment and rehabilitation programs for patients with respiratory or cardiovascular conditions.
Po2 and Sleep
During sleep, Po2 levels can fluctuate due to changes in respire patterns and oxygen demand. In healthy individuals, these fluctuations are commonly minor and do not regard oxygenation status. However, in individuals with sleep disarray suspire, such as clogging sleep apnea (OSA), Po2 levels can drop importantly during apneic episodes.
Obstructive sleep apnea is a common condition qualify by repeated episodes of amphetamine airway obstruction during sleep, star to intermittent hypoxemia and hypercapnia. This can result in a decrease in Po2 levels and an increase risk of cardiovascular and metabolic complications.
Monitoring Po2 levels during sleep can help diagnose sleep unhinge breathing and guide treatment. Continuous positive airway pressure (CPAP) therapy is a common treatment for OSA that helps keep unfastened airways and prevent apneic episodes, thereby improving oxygenation and Po2 levels.
In drumhead, realize the normal value of Po2 and its clinical significance is all-important for contend respiratory and cardiovascular health. Po2 measurements provide valuable info about oxygenation status and can guidebook treatment decisions in various clinical settings. Regular monitoring of Po2 levels is essential for guarantee adequate oxygen delivery to the body's tissues and for prevent complications connect with hypoxemia.
Po2 levels can be influenced by several factors, including altitude, age, respiratory diseases, and cardiovascular health. Interpreting Po2 measurements requires consideration of these factors and the patient's clinical context. Oxygen therapy is a mutual intervention used to increase Po2 levels in patients with hypoxemia, and regular monitoring of Po2 levels is all-important for deal respiratory conditions.
Po2 levels can also be affected by exercise and sleep, and monitor these levels during these activities can provide worthful info about respiratory and cardiovascular function. In individuals with sleep disordered breathing, Po2 levels can drop importantly during apnoeic episodes, starring to an increase risk of complications. Monitoring Po2 levels during sleep can facilitate diagnose sleep disquiet breathing and guide treatment.
to summarize, Po2 is a critical measurement in respiratory physiology and clinical medicine. Understanding the normal value of Po2 and its clinical significance is all-important for managing respiratory and cardiovascular health. Regular monitor of Po2 levels and conquer rendition of these measurements can guide treatment decisions and improve patient outcomes.
Related Terms:
- po2 blood test entail
- normal po2 levels in kpa
- causes of eminent po2
- high po2 tier meaning
- po2 in medical terms
- eminent po2 means what